Medication errors by patients and caregivers – strategies for pharmacists
By Dorothy Li, B.Sc.(Pharm), CSPI, BC Drug and Poison Information Centre
Reviewed by C. Laird Birmingham, MD, MHSc, FRCPC
Acknowledgement: Victoria Wan, Biostatistician for BC Centre for Disease Control
A version of this article was originally published in the BC Pharmacy Association’s March 2019 Tablet magazine.
A review of pharmacy’s most common patient-induced therapeutic errors and how pharmacists can help avoid them by the BC Drug and Poison Information Centre.
Pharmacists routinely deal with medication errors (MEs), which often occur during medication prescribing and dispensing. Safe dispensing includes use of the “5 rights” pneumonic: right patient, medication, dose, route and time/way. (1, 2) But many MEs occur after our patient leaves with a correctly prescribed and dispensed medication. This article discusses how patients commit MEs and what pharmacists can do to reduce them.
Medication errors in BC
Every month, the BC Drug and Poison Information Centre (DPIC) receives on average 230 calls regarding MEs occurring at home. In 2018, this represented 9.7% of total calls. The majority (97%) were patient or caregiver initiated errors: 66% in adults, 30% in children 0-12 years and 4% in adolescents. There were no reported deaths, although 15% were referred/presented to Health Care Facilities (HCF)* and 5.3% had moderate or major effects. Of adults ≥ 60 years, 23% were referred/presented to HCF. Most common MEs in all age groups were: wrong medication given/taken, medication given/taken twice and other incorrect dose. Additional common MEs in children ≤ 5 years were: confused units of measure and incorrect formulation/concentration administered. The top drug classes were analgesics, cardiovascular drugs, antidepressants and hormones (insulin, oral hypoglycemics, biguanides and thyroid preparations). (3)
(See Figure 1 and Table 1 for ME classification and specific examples)
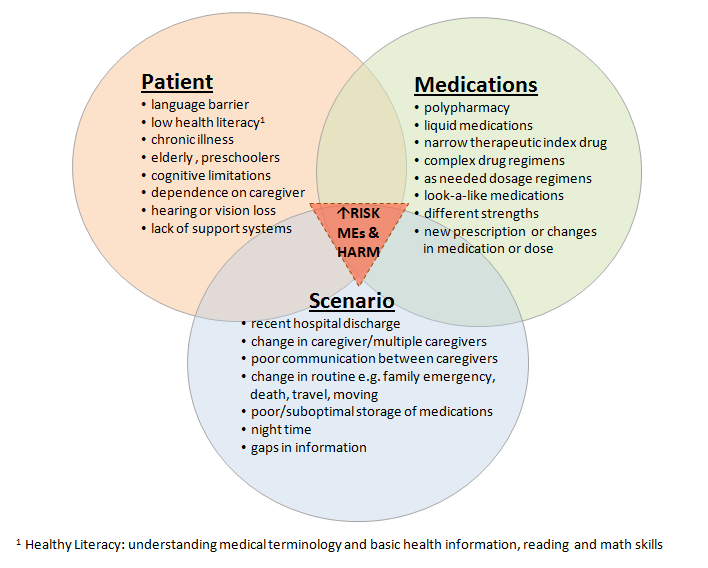
Figure 2: Risks for medication errors: Patients, medications and scenarios (2,6,10, 21-23, 31-36)
“Double dosing” medication errors
An adolescent accidentally took 600 mg of bupropion XL and was referred to the emergency. She had been taking 2 x 150 mg tablets for one month. Following a switch to 300 mg tablets, she erroneously took 2 tablets, out of habit. A seizure occurred at 11 hours. This patient had no known risk factors for seizure except the double dose of bupropion, a narrow therapeutic index (NTI) drug. She knew how to take her medication but made a slip or “action-based error.” (4)
Drug shortages, which can necessitate changes in medication strength, may place patients at risk for double doses. Heightened awareness coupled with careful counselling on the potential effects of double doses for NTI drugs may prevent similar MEs.
Among 876 double doses reported to U.S. poison control centers from 2006 to 2015, life-threatening symptoms occurred in 12 cases (1%): bupropion or tramadol – seizures; beta-blockers or calcium channel blockers – bradycardia, hypotension and heart block; and propafenone – ventricular tachycardia. With intensive care, all recovered. Moderate effects occurred in 206 (25%) cases, most commonly with calcium channel blockers, beta blockers, alpha-2 agonists, amphetamines, antidepressants, atypical antipsychotic, analgesics, insulin and sulfonylureas. (5) While this double dose study reported no deaths, a larger U.S. study of MEs including all types of errors occurring outside of hospitals reported a death rate of 0.02%. (6)
“Knowledge-based” medication errors
Two weeks after a new prescription for methotrexate and prednisone, a patient in her 90s presented to the emergency with profound mucositis. Misunderstanding the instructions, she took 5 mg of methotrexate orally each day (rather than once weekly as prescribed). She received IV leucovorin, filgrastim (G-CSF) and a blood transfusion for pancytopenia. Morphine and nasogastric feeds treated her mouth pain and dysphagia. By day 21, she was able to eat for the first time.
Advanced age, polypharmacy, new prescriptions and complex drug regimen of an NTI drug were risks for this ME. This error was “knowledge-based,” resulting from not understanding how to safely take her weekly methotrexate and the dangers of daily dosing. (4) Strategies to avoid this type of ME include careful counselling using the teach-back technique and encouraging questions by asking “Do you have any concerns about your medication?” The Institute of Safe Medicine Practice further recommends limiting methotrexate quantity to 4 weeks, folate supplementation, regular laboratory monitoring and specifying a particular day of the week in the directions. (7-9)
Methotrexate MEs resulting in life-threatening effects is not a new problem. (10,11) Life-threatening pancytopenia and death occurs with as little as 3 days of consecutive dosing or a cumulative dose of 40 mg. (10,12,13) The case above was one of 66 reported to DPIC over 7 years. The majority of these cases occurred at home (92%). The most common errors were: daily instead of weekly dosing (29%), doses too close together (27%) and incorrect amount (24%). Many patients were referred/presented to hospital (42%) and received intravenous leukovorin (24%) and G-CSF (8%). Risk factors included: new prescription, dose or route change, or complicated regimen (36%); elderly (32%), polypharmacy and multiple disease states (29%). Isolated cases involved communication problems (language or hearing) and cognitive issues. (14)
“Action-based” medication errors
A woman in her late 60’s called DPIC at 10 PM from her home after injecting 60 units of short-acting insulin instead of her long-acting insulin. Her husband was with her and became aware of the error. DPIC guided management at home with additional carbohydrate and protein intake & frequent blood sugar monitoring. Symptoms and management of hypoglycemia were discussed. Close follow-up by DPIC during the critical period allowed safe management at home without hypoglycemia. This patient knew how to take her insulin. She made a slip or “action-based” error by picking up the wrong insulin pen. This error could also be considered a “rule-based” error i.e. if the rule was to double check the type of insulin pen before administration, the error occurred because the rule was not followed.
Insulin deserves heightened attention since errors in dosing or type of insulin have resulted in severe hypoglycemia and death. (15-17). Administering rapid or short-acting insulin instead of long-acting insulin in the evening is the most common scenario reported to DPIC. In 2018 DPIC received 240 calls about insulin errors that occurred at home. The majority (82 %) were managed at home with telephone guidance by DPIC with a good outcome. The remainder were referred to or had already presented to hospital. Causes of hospital referral included: hypoglycemia not responding to treatment with oral glucose or food, inadequate support at home (e.g. patient is alone), insufficient food or glucose available to treat hypoglycemia or insufficient blood sugar monitoring strips available. Giving rapid-acting insulin in error is more likely to result in hypoglycemia than giving long-acting insulin in error. (18) Risk factors for insulin administration errors include: evening dosing, new insulin user, drug regimen changes or complex regimen, similar appearance of pen devices and poor vision. (18,19) The risk of error is increased during the evening when patients may be tired/less alert or if they are switching from short acting insulin during the day to long-acting insulin in the evening. Management of insulin errors in the evening can be complicated because this is the time patients are tired and getting ready for sleep.
Prevention
The majority of MEs at home do not cause injury. A few result in major clinical complications and some in death. (3, 20, 21) The pharmacist’s goal is to reduce harm associated with MEs. (22-25) Regulatory strategies have effectively reduced MEs with cough and cold preparations in preschoolers. (20) Proven front-line strategies include: pill organizers, improved patient information, helping patients calculate and measure liquid doses, active participation in treatment by patients, encouraging questions to resolve doubts, motivational interviewing technique and phone apps. (9,21)
The role of the pharmacist in medication safety goes beyond the “5 rights.” By identifying patients, medications and scenarios that have an elevated risk of ME the pharmacist can tailor ME prevention strategies during the process of pharmaceutical care, dispensing and counselling (see Figures 1 & 2). For NTI drugs, extra care in counselling at-risk patients and using teach-back technique to determine the patient’s level of understanding is essential. In case of inadvertent ME, call the Poison Control Centre for immediate risk assessment, recommendations and management.
*HCF = mostly hospitals, also physician’s offices and medical clinics
(See Figures 1 and 2 for MEs classification, prevention and risk assessment. See Supplement 1 below for explanation of teach-back technique.)
Figure 1: Medication error classification and prevention (2,4,6,9,21-23,26-31)
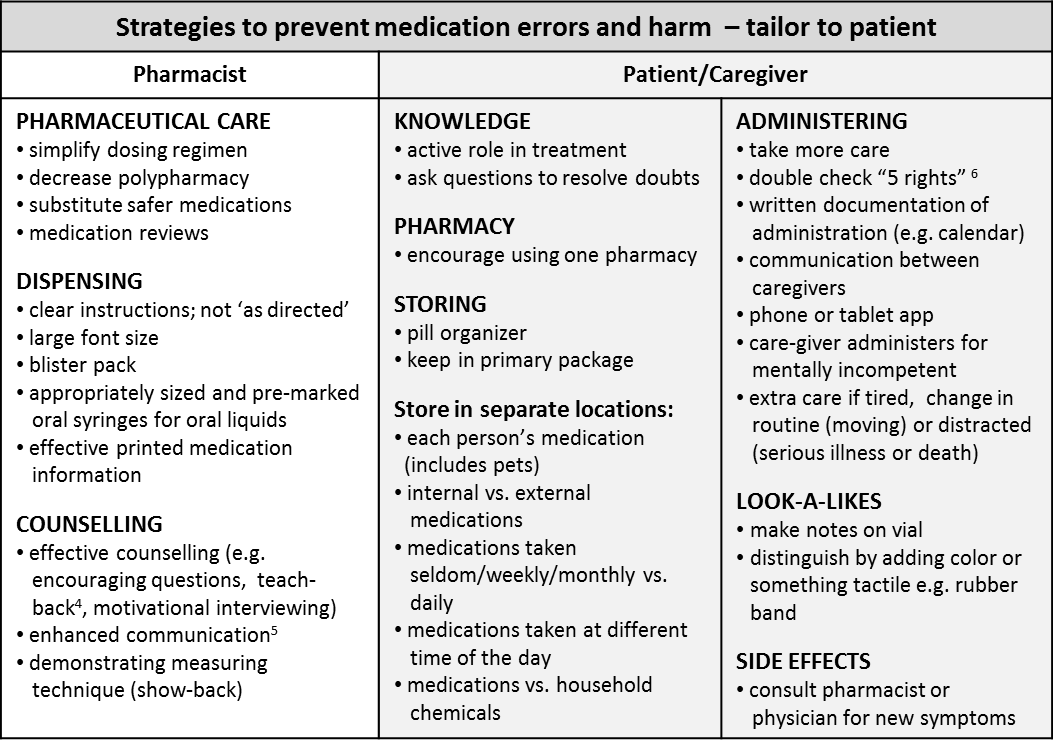
Table 1: Top Scenarios of MEs occurring at home with selected examples (% of MEs in 2018)
- Took/gave wrong medication (26%).
Adult female accidently used her antifungal/steroid ear drops in her eyes then developed bloodshot and painful eyes despite flushing eyes for 20 minutes. Referred to emergency department.
Adult in his 60’s accidently swallowed his vial of “spare meds” instead of the vial containing his night time meds. “Spare meds” included extra doses of ramipril, acetaminophen, bisoprolol and ASA. Referred to emergency department for cardiac monitoring.
- Took/gave medication twice (25%)
2-year-old was given dose of acetaminophen elixir by Dad. Dose repeated in 30 minutes by Mom. No treatment needed.
Female in her 70’s took an extra dose of warfarin in the evening. She took her dose at 8 PM, then daughter organized her medications for the evening for the next day and Mom also took those. No treatment needed.
- Incorrect dose (16%)
Male in his 70’s took a double dose of glyburide and metformin at suppertime. Blood sugar dropped to 2.7. Referred to emergency department
Adult male accidently took 4 x ranitidine 150 mg instead of 1 tablet. He mixed up the amount because he usually takes 4 tablets of quetiapine. Patient was managed at home.
- Took/gave doses too close together (10%)
Dad gave 7-year-old son 200 mg of ibuprofen instead of acetaminophen which they were instructed to give alternatively by the doctor. Previous dose of ibuprofen was given 3 hours ago. No treatment needed.
- Took/gave someone else’s medication (5.3%)
Female in her 40’s accidently took her husband’s ticagrelor 2 x 80 mg. No treatment needed.
An adult accidently took his dog’s oclacitinib 16 mg. No treatment needed.
- Confused units of measure (5%)
An adult accidently took 2 tablespoon instead of 2 teaspoon of cough syrup containing dextromethorphan, pseudoephedrine and guaifenesin. Patient was managed at home and advised of potential side effects and to avoid further cough syrup for 12 hours
- Incorrect route (4%)
Healthy adult female self-administered clotrimazole 200 mg orally instead of vaginally. Judged as non toxic. Recommended food and drink.
Adult female took two dimenhydrinate suppositories by mouth. No treatment needed.
Adult swallowed his tiotropium inhalation capsules. Judged as non toxic. Caller was advised to take a dose by inhalation.
Supplement 1: Teach-back method for enhancing patient understanding of medication information (37-44)
The goal of counselling is that the patient understands how to take their medications properly. This promotes adherence and optimizes safety. The pharmacist may believe the information they provided was clear, but the only way to know for sure is to ask the patient what they understood. The teach-back method does this. It is used to validate the patient’s understanding and decide if more explanation is needed. This method of communication improves medication adherence, reduces medication errors and improves health outcomes.
Using the teach-back method, the patient is given information and then asked to explain back in their own words what they need to know or do. Careful phrasing of the teach-back question helps the patient understand the purpose and that they are not being ‘tested’. Example teach-back questions include: “To be sure that I have explained everything correctly, could you tell me how and when you will take your medication?” “Would you mind showing me how you are going to use your inhaler to make sure that I was clear with my instructions?” “I want to make sure I was clear about the side effects of this medication. Can you tell me what you will be watching out for?” “To be sure I have covered all the important points on safe medication storage to prevent errors, can you tell me how you will be storing your medication when you get home?”
If misunderstanding or information gaps are identified, the pharmacist re-phrases the information or uses diagrams, teaching aids, or demonstrations to help the patient understand. Careful wording at this stage continues to keep the patient in a mindset open for learning. For example, “I don’t think I was clear enough on explaining about the side effects of this medication ...“ After re-explaining, patient understanding is checked again. This process is continued until understanding is demonstrated. If the patient does not understand after a number of cycles, other strategies are used.
It’s best to choose the most important points for teach-back since most people only remember a few points at one time. Teach the first concept in 2-3 manageable points, then check for understanding. Once understanding of the first concept is confirmed, move onto the next concept. In the teach-back model, this is referred to as “chunk and check”. Addressing the most important concept first may enhance recall of that piece of information.
Teach-back allows for dialogue between the pharmacist and the patient, enhancing patient engagement and trust. As a pharmacist, this technique will help you discover which explanations and other communication aids are best understood by patients. Clinicians who practice teach-back regularly find that they have become more effective at teaching and it only takes minimal extra time.
Teach-back may be used for any medication counselling but is strongly recommended for new medications, changes in doses, high risk drugs and complex drug regimens; and for patients with chronic diseases, who are elderly or where there are concerns about health literacy; and during transitions between health care settings.
To learn more about how to use teach-back in your practice, work through the following online Teach-back modules:

BC DRUG AND POISON INFORMATION CENTRE
The BC Drug and Poison Information Centre (DPIC) was established in 1975 through the cooperative efforts of the Hospital Programs Branch of the BC Ministry of Health and the Faculty of Pharmaceutical Sciences at the University of British Columbia (UBC). It is located at the BC Centre for Disease Control in Vancouver and is staffed with pharmacists, nurses, and physicians who have specific expertise in the provision of drug and poison information services.
The original mandate of the Centre called for the development of centralized services to assist health professionals throughout BC in providing optimal levels of drug therapy and poison management. Considerable progress has been made in this respect through expansion of DPIC programs over the ensuing years. Notably, the Centre has assumed provision of poison information services to the BC public, a population of approximately 4.4 million.
Guest Post Disclaimer
ReadLinks Guest Posts are intended to expose the public and pharmacy professionals to a diverse range of knowledge, and expertise, with the goal of expanding awareness of issues related to public safety and pharmacy practice. While the College enforces strict Guest Post Submission Guidelines, the views and opinions expressed in Guest Posts articles are those of the author(s) and do not necessarily reflect the official standards or positions of the College of Pharmacists of British Columbia.
References
1. Practice Review Program. Practice tools for safe drug therapy. [Document on the Internet]. Available at: http://www.bcpharmacists.org/library/5_Programs/5-2_PRP/5222-PRP_Support_Tool_Safe_Drug_Therapy.pdf. Accessed January 9, 2019.
2. Practice Review Program. Counselling. BC College of Pharmacists. [Document on the internet]. Available at:. http://www.bcpharmacists.org/readlinks/prepare-your-next-practice-review.... Accessed January 9, 2019.
3. Li D, Wan V. Analysis of therapeutic errors reported to BC Drug and Poison Information Centre. January 2012 to December 2018. Data on file. January 9, 2019.
4. Ferner RE, Aronson JK. Clarification of terminology in medication errors. Definitions and classification. Drug Safety. 2006;29(11):1011-1022.
5. Correia MS, Whitehead E, Cantrell FL, Lasoff DR, Minns AB. A 10-year review of single medication double-dose ingestions in the nation's largest poison control system. Clin Toxicol (Phila). 2019;57(1):31-35. doi: 10.1080/15563650.2018.1493205.
6. Shah K, Barker KA. Out-of-hospital medication errors: a 6-year analysis of the national poison data system. Pharmacoepidemiol Drug Saf. 2009;18(11):1080-1085. doi: 10.1002/pds.1823.
7. Pharmacy Matters. Severe Harm and Deaths Associated with Incidents Involving Low-dose Methotrexate. Pharmacy Matters. 2015;40(6) [Document on the internet]. http://www.bcpharmacists.org/readlinks/pharmacy-matters-severe-harm-and-... Accessed January 13, 2019.
8. ISMP. Call to Action: Longstanding strategies to prevent accidental daily methotrexate dosing must be implemented. ISMP Institute for Safe Medication Practices. August 9, 2018. [Page on the Internet]. https://www.ismp.org/resources/call-action-longstanding-strategies-preve.... Accessed January 13, 2019.
9. Nunes V, Neilson J, O’Flynn N, Calvert N, Kuntze S, Smithson H, Benson J, Blair J, Bowser A, Clyne W, Crome P, Haddad P, Hemingway S, Horne R, Johnson S, Kelly S, Packham B, Patel M, Steel J (2009). National Collaborating Centre for Primary Care (UK). Medicines Adherence: Involving Patients in Decisions About Prescribed Medicines and Supporting Adherence [Internet]. London: Royal College of General Practitioners (UK); 2009 Jan. (NICE Clinical Guidelines, No. 76.) (Document on the internet) Available from: https://www.ncbi.nlm.nih.gov/books/NBK55440/ Accessed: January 13, 2019.
10. Cairns R, Brown JA, Lynch AM, Robinson J, Wylie C, Buckley NA. A decade of Australian methotrexate dosing errors. Med J Aust. 2016;204(10):384.
11. Arnet I, Bernhardt V, Hersberger KE. Methotrexate intoxication: the Pharmaceutical Care process reveals a critical error. J Clin Pharm Ther. 2012;37(2):242-244. doi: 10.1111/j.1365-2710.2011.01263.x.
12. Hocaoglu N, Atilla R, Onen F, Tuncok Y. Early-onset pancytopenia and skin ulcer following low-dose methotrexate therapy. Hum Exp Toxicol. 2008;27(7):585-589. doi: 10.1177/0960327108094507.
13. Vial T, Patat AM, Boels D, Castellan D, Villa A, Theophile H, et al. Adverse consequences of low-dose methotrexate medication errors: data from French poison control and pharmacovigilance centres. Joint Bone Spine. 2019;86:351-355. https://doi.org/10.1016/j.jbspin.2018.09.006.
14. Li. D, Retrospective Review of methotrexate calls to the BC Drug and Poison Information Centre September 2011 to December 2018, Data on file. January 9, 2019.
15. Magal P, Spiller HA, Casavant MJ, Chounthirath T, Hodges NL, Smith GA. Non-health care facility medication errors associated with hormones and hormone antagonists in the United States. J Med Toxicol. 2017;13(4):293-302. doi: 10.1007/s13181-017-0630-8.
16. ISMP Canada. Deaths associated with medication incidents occurring outside regulated heatlhcare facilities. ISMP Canada Safety Bulletin. 2014;14(2):1-8. [document on the internet]. Available at: https://www.ismp-canada.org/download/safetyBulletins/2014/ISMPCSB2014-2_.... Accessed May 2, 2019.
17. WHO . Reporting and learning systems for medication errors: the role of pharmacovigilance centres. 2014. [document on the internet]. Available at: http://apps.who.int/medicinedocs/documents/s21625en/s21625en.pdf. Accessed May 2, 2019.
18. Cumming E, Li R, Durigon M, Omura JD, Elliott T, Kosatsky T. The who, when and why of unintentional insulin errors as documented by poison centre help calls: a cross-sectional study. 2018. Data on file.
19. Grissinger M, Gaunt MJ. Reducing harm in patients using insulin. Consult Pharm. 2014;29(5):290-302. doi: 10.4140/TCP.n.2014.290.
20. Brophy TJ, Spiller HA, Casavant MJ, Chounthirath T, Smith MD, Xiang H. Medication errors reported to U.S. Poison Control Centers, 2000–201. Clin Toxicol (Phila). 2014. 52(8):880-888. doi: 10.3109/15563650.2014.953168.
21. Mira JJ, Lorenzo S, Guilabert M, Navarro I, Pérez-Jover V. A systematic review of patient medication error on self-administering medication at home. Expert Opin Drug Safety. 2015;14(6):815-838. doi: 10.1517/14740338.2015.1026326.
22. Hodges NL, Spiller HA, Casavant MJ, Chounthirath T, Smith GA. Non-health care facility medication errors resulting in serious medical outcomes. Clin Toxicol (Phila). 2018. 56(1):43-50. doi: org/10.1080/15563650.2017.1337908.
23. Taylor DM, Robinson J, MacLeod D, MacBean CE, Braitberg G. Therapeutic errors involving adults in the community setting: nature, causes and outcomes. Aust N Z J Pub Health. 2009;33(4):388-394. doi: 10.1111/j.1753-6405.2009.00413.x.
24. Ferner RE, Aronson JK. Preventability of drug-related harms - Part I: a systematic review. Drug Saf 2010;33(11):985-994. doi: 10.2165/11538270-000000000-00000.
25. Ferner RE. An agenda for UK clinical pharmacology medication errors. Br J Clin Pharmacol. 2012;73(6):912-916. doi:10.1111/j.1365-2125.2012.04236.x
26. Yin HS, Dreyer BP, Moreira HA, van Schaick L, Rodriguez L, et al. Liquid medication dosing errors in children: role of provider counseling strategies. Acad Pediatr. 2014;14(3):262-270. doi: 10.1016/j.acap.2014.01.003.
27. Madlon-Kay DJ, Mosch FS. Liquid medication dosing errors. J Fam Pract. 2000;49(8):741-4.
28. Hayes BD, Klein-Schwartz W, Gonzales LF. Causes of therapeutic errors in older adults: evaluation of National Poison Centre Data. J Am Geriatr Soc. 2009;57(4):653-658. doi: 10.1111/j.1532-5415.2008.02166.x.
29. Naunton M, Nor K, Bartholomaeus A, Thomas J, Kosari S. Case report of a medication error. In the eye of the beholder. Medicine. 2016;95(28):e418. doi.org/10.1097/MD.0000000000004186.
30. Kimminau MD. Spoons provide potential for dosing errors. Am Pharm. 1979;19 (12):25-27.
31. Field TS, Mazor KM, Briesacher B, DeBellis KR, Gurwitz JH. Adverse drug events resulting from patient errors in older adults. J Am Geriatr Soc. 2017;55:271-276.
32. Shane R, Amer K, Noh L, Luong D, Simons S. Necessity for a pathway for "high-alert" patients. Am J Health Syst Pharm. 2018;75(13):993-997.
33. Yin HS, Parker RM, Sanders LM, Mendelsohn A, Dreyer BP, Bailey SC, et al. Pictograms, units and dosing tools, and parent medication errors: a randomized study. Pediatrics. 2017;140(1):e20163237. doi: 10.1542/peds.2016-3237.
34. Crouch BI, Caravati EM, Moltz E. Tenfold therapeutic dosing errors in young children reported to US poison control centres. Am J Health Syst Pharm. 2009;66(14):1292-1296. doi: 10.2146/080377.
35. Moore TJ, Walsh CS, Cohen MR. Reported medication errors associated with methotrexate. Am J Health Syst Pharm. 2004;61(13):1380-1384.
36. Singh A, Handa AC. Medication Error - a case report of misadventure with methotrexate. JNMA J Nepal Med Assoc. 2018;56(211):711-715.
37. Brega AG, Barnard J, Mabachi NM, Weiss BD, DeWalt DA, Brach C, Cifuentes M, Albright K, West, DR. AHRQ Health Literacy Universal Precautions Toolkit, Second Edition. (Prepared by Colorado Health Outcomes Program, University of Colorado Anschutz Medical Campus under Contract No. HHSA290200710008, TO#10.) AHRQ Publication No. 15-0023-EF. Rockville, MD. Agency for Healthcare Research and Quality. January 2015. [Document on the internet]. Available at:. https://www.ahrq.gov/sites/default/files/wysiwyg/professionals/quality-p... Accessed: May 2, 2019.
38. Always use teach-back! Training toolkit. [website]. Available at: www.teachbacktraining.org Accessed May 2, 2019.
39. Teach-back. [Website]. Sydney, NSW: South Eastern Sydney Local Health District, Deakin University Accessed May 2, 2019.
40. Dinh TTH, Bonner A, Clark R, Ramsbotham J, Hines S. The effectivenss of the teach-back method on adherence and self-management in health education for people with chronic disease: a systematic review. JBI Database System Rev Implement Rep. 2016;14(1):210-247. doi: 10.11124/jbisrir-2016-2296.
41. Beauchamp A, Batterham RW, Dodson S, Astbury B, Elsworth GR, McPhee C, et al. Systematic development and implementation of interventions to Optimise Health Literacy and Access (Ophelia). BMC Public Health. 2017;17:230-248. doi: 10.1186/s12889-017-4147-5.
42. Abrams MA, Kurtz-Rossi S, Riffenburgh A, Savage B. Building Health Literate Organizations: A Guidebook to achieving organizational change. 2014. [Document on the internet]. Available at:. https://www.hrhresourcecenter.org/node/5890.html Accessed May 18, 2019.
43. Batterham RW, Hawkins M, Collins PA, Buchbinder R, Osborne RH. Health literacy: applying current concepts to improve health services and reduce health inequalities. Public Health. 2016;132:3-12. doi: 10.1016/j.puhe.2016.01.001.
44. AHRQ. Health Literacy Universal Precautions Toolkit, 2nd Edition. [Website]. Available at:. https://www.ahrq.gov/professionals/quality-patient-safety/quality-resour... Accessed May 27,2019.
- Guest Post
 Share
Share


